Phalloplasty is a complicated, multi-stage surgery to create a penis-like structure that combats Gender Dysphoria in transgender men. The desired outcome and functionality can be chosen by the patients and there are several techniques used. There are no gold standards or correct technique when performing the surgery, though depending on what the desired goals there are more widely used options. Patient goals may include:
- Phallic shaft creation: sculpting the shaft of a penis using donor tissue.
- Penile urethroplasty: creating a longer urethra using donor tissue, allows for urination through the tip of the penis.
- Perineal urethroplasty: lengthening the urethra and creating a permanent opening at the base of the penis.
- Perineoplasty: tightening the muscles between the anus and vulva.
- Scrotoplasty: creation of a scrotum.
- Vaginectomy: removal of the vagina and closing of the vaginal opening.
- Hysterectomy and Oophorectomy: removal of the uterus and ovaries.
- Galvanoplasty: sculpting the head of the penis.
- Testicular implants: implants to fill a created scrotum.
- Erectile device: internal or external devices that allow for erections and penetrative intercourse.
Some patients may want all these surgeries. Others may only opt for a few. It is important to keep in mind that each of these induvial surgeries come with their own set of complications and recovery time. Each surgery can be performed using a variety of techniques depending on: the body type of the patient, what the patient’s goals are, and what the surgeon deems most appropriate. The more complicated the surgery becomes, the higher the risk of complications becomes.
Before starting the surgery there are choices that a patient must make. First, is if the patient would like to be able to urinate from the tip of the phallus, having to elongate the urethra increases risk of complication. Though, the urethra may be extended to the bass of the phallus with more ease and allows for later elongation for future transition surgeries. If the patient would like to urinate from the tip of their phallus. Then their urethra needs to be lengthened and attached to the urethra housed in the shaft. A vaginectomy with urethra lengthening to only the base of the phallus has been linked to lower risk of complication and is the recommended route.
The phallus is created from donor tissue and will be about 5-6 inches long. Length does vary depending on body type and will shrink after the swelling from the surgery subsides. The donor site should be thin and hairless. If there is hair, it will be removed via laser or electrolysis. Areas of skin that have been scared may compromise reliable blood supply and are not advisable to be used. Also, consider the skin elasticity, body fat distribution, and size of the patient. It is noted that a BMI less than 30 is ideal, and above 35 creates a longer distance to the urethra, making the surgery more difficult. Obesity adds to possible risk when performing phalloplasty.
Pre-Operation
Most importantly, a pre-op psychosocial assessment may be necessary before being accepted. Most surgical centers will require two letters of recommendation as well as well-documented Gender Dysphoria. The patient must also have a post-op care plan in place. Phalloplasty will limit mobility, work, travel, bathing, intimacy and create plenty of post-op appointments for the first 1-2 months after surgery.
Donor Tissue Selection
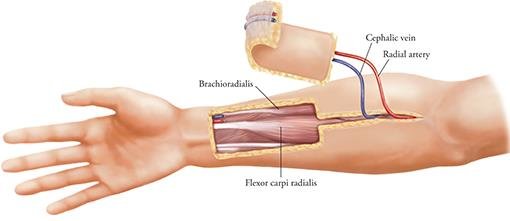
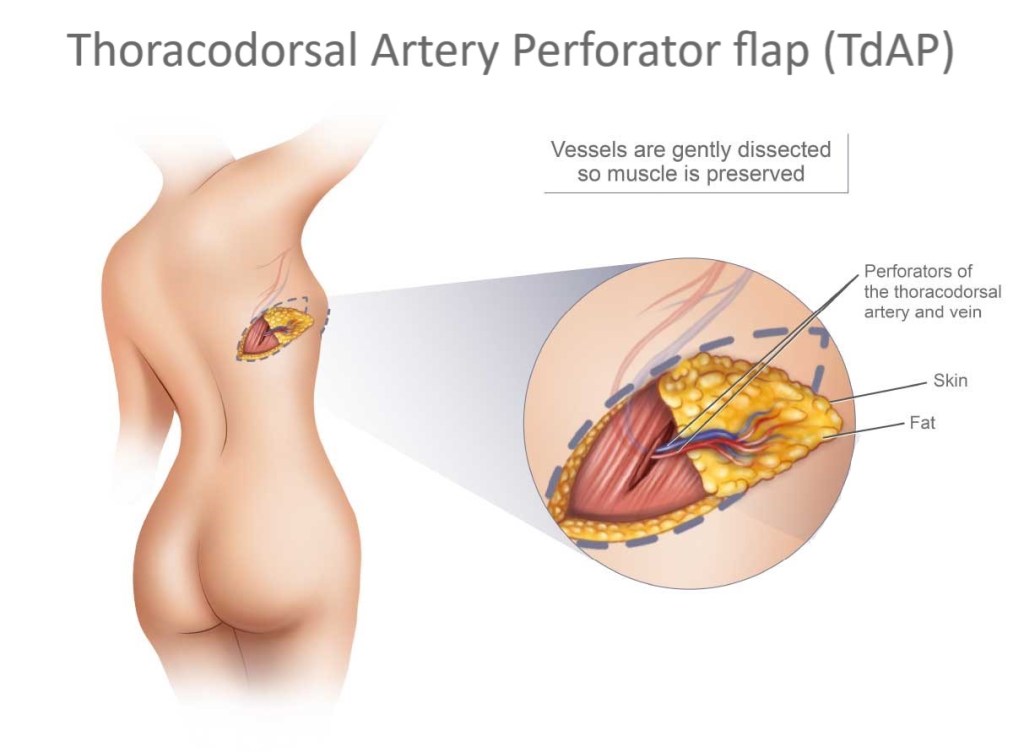
As for flap options to use to create the shaft, if the patient does not want to urinate through the tip of the phallus, then a shaft-only design will be used. Donor tissue for a shaft-only phallus can come from: the anterolateral thigh (ATL), radial forearm free flap (RFFF), superficial circumflex iliac artery perforator flap (TdAP), or the thoracodorsal artery perforator flap. If the patient does wish to have phallic urination, the most widely used design is the tube within a tube (TWT). The TWT design consists of two skin paddles that are rolled in opposite directions. Another option to gain phallic urination is a composite flap where the urethra and shaft are from separate donor sites.
anterolateral thigh (ATL):
radial forearm free flap (RFFF):
superficial circumflex iliac artery perforator flap (SCIP):

thoracodorsal artery perforator flap (TdAP):
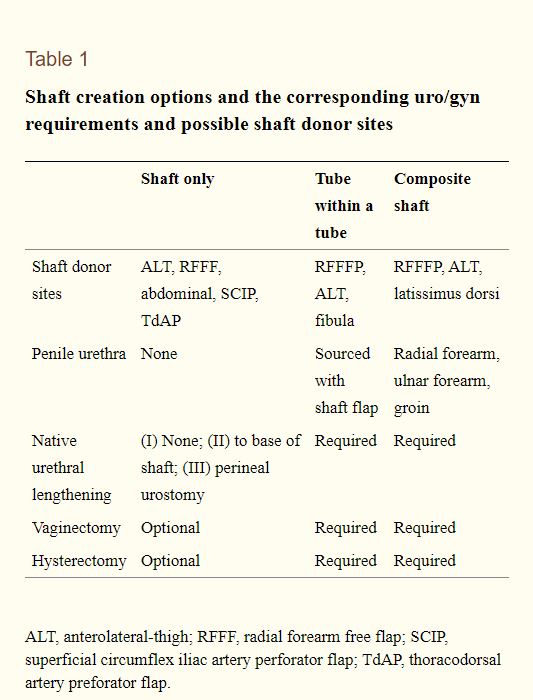
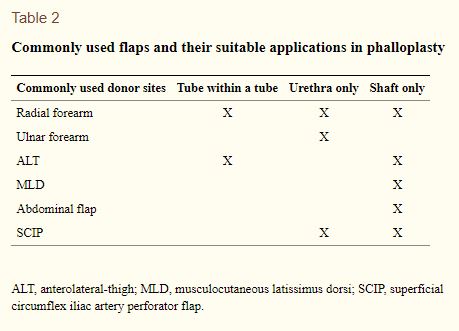
Depending on the needs of the patient and whether the donor sites will be used for: a TWT, urethra only, or shaft-only; Will determine where the donor tissue will be taken from. Below are charts for commonly used flaps (Table 2) and shaft creation options and the corresponding requirements (table 1), both tables were provided by Translational Andrology and Urology (Heston, Esmonde, Dugi III, & Berli, 2019).
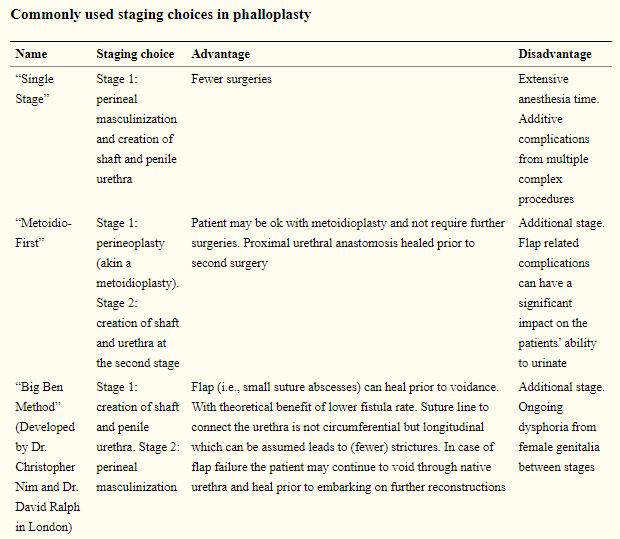
Finally, there are three commonly used staging choices in phalloplasty. Depending on the needs of the patient, and any further surgeries for further transition, one of these three staging choices will likely be used. There are advantages and disadvantages to each choice, and discussion with providers is needed to help understand what choice the best match may be.
Sources
Heston, A. L., Esmonde, N. O., Dugi III, D. D., & Berli, J. U. (2019). Phalloplasty: Techniques and outcomes. Translational Andrology and Urology, 8(3), 254-265. doi:10.21037/tau.2019.05.05
Levine, J., Dr. (2021). Thoracodorsal Artery Perforator (TDAP) Flap [Digital image]. Retrieved 2021, from https://centerforbreastreconstruction.com/before-and-after-breast-reconstruction-photos-tdap-i
https://plasticsurgerykey.com/. (2019). Technique of Flap Harvest [Digital image]. Retrieved 2021, from https://plasticsurgerykey.com/groin-flap-and-superficial-circumflex-iliac-artery-perforator-flap/
Awny, Shadi. (2019). Anterolateral thigh versus radial forearm free flaps in reconstruction of oral cavity malignant defects. 10.13140/RG.2.2.33768.01288.
NJ, B., SC, L., & M, S. (2013). Trans-vastus Intermedius Transfer of the Pedicled Anterolateral Thigh Flap for Posterior Thigh Reconstruction. [Digital image]. Retrieved 2021, from https://openi.nlm.nih.gov/detailedresult?img=PMC4174101_gox-1-e81-g001&req=4
Ercolano, A. (2021, January 26). FAQ: Phalloplasty: The Johns Hopkins Center for Transgender health. Retrieved February 15, 2021, from https://www.hopkinsmedicine.org/center-transgender-health/services-appointments/faq/phalloplasty#patient-process