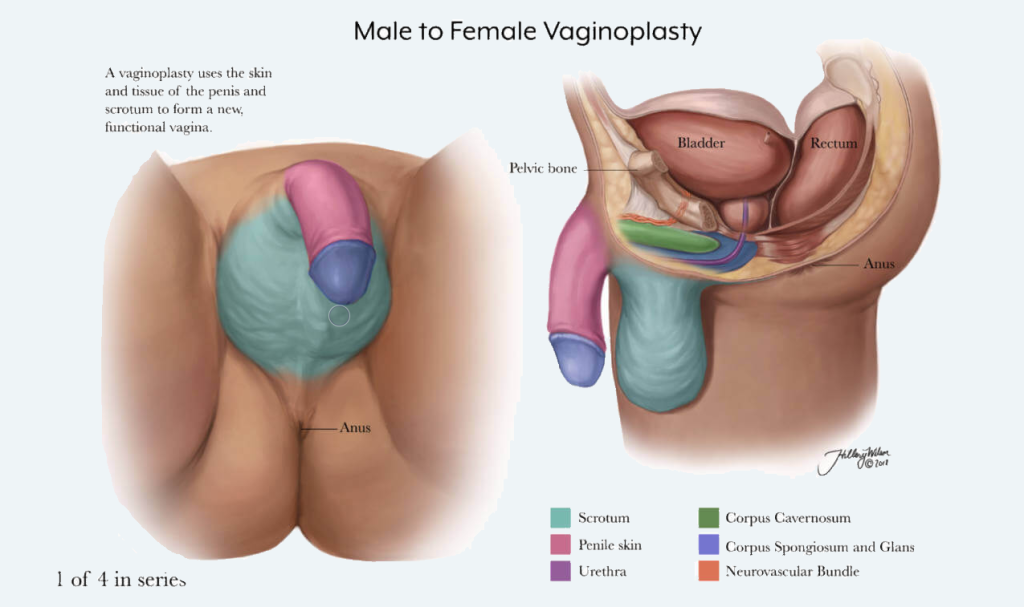
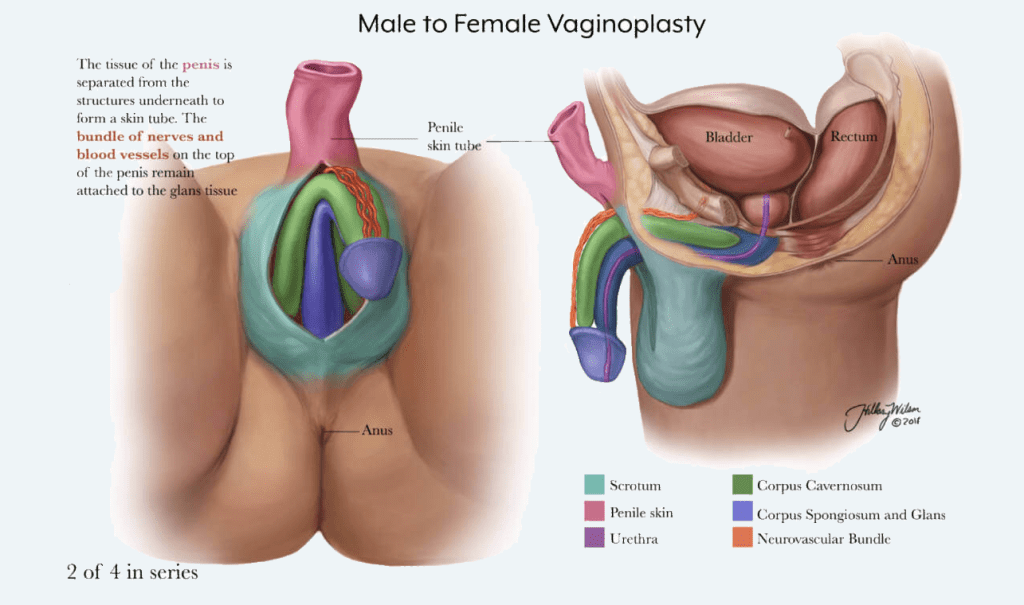
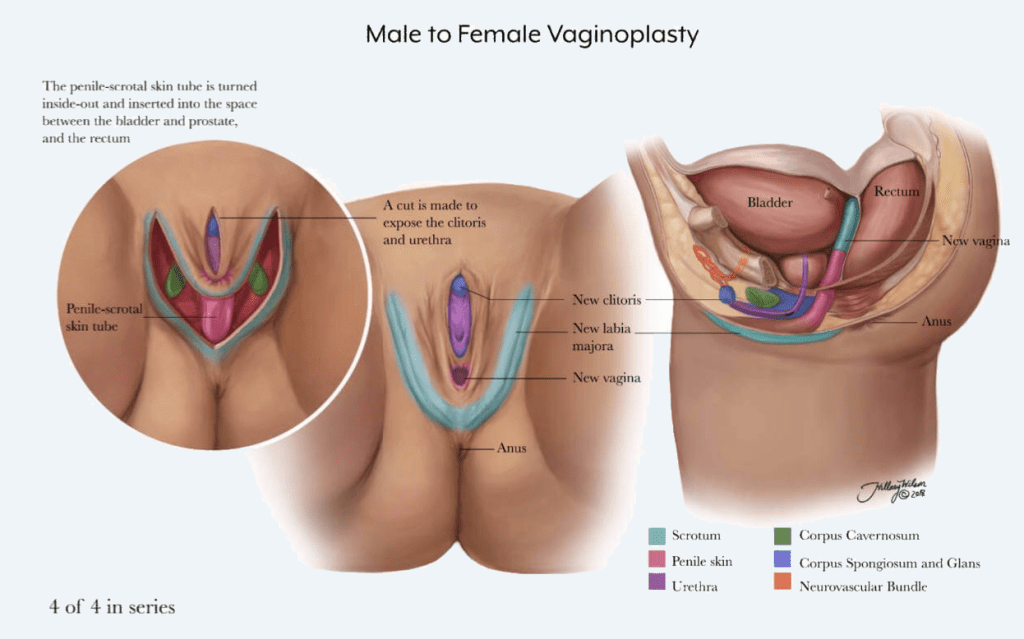
Vaginoplasty is a complex, single-stage, surgical process where the male genitalia is removed and used to create a vaginal opening. The most common technique used is the penile inversion procedure. Using this technique the vaginal opening is created between the rectum and urethra. The vaginal lining is created from penile skin, the labia majora is created using scrotal skin, and the clitoris is created from the glans penis. The prostate is left in place to avoid complications and acts as the anatomic equivalent to the ‘g-spot.’ If extra skin is needed, skin grafts from the thigh or abdomen are used, though skin from these locations do not have as much feeling as skin already on the genitalia. Some patients opt for a second surgery to add more skin to the clitoral hood or labia majora making them appear more natural.
Another less common technique is using the colon instead of penile skin to create the vaginal opening. This technique is limited in use and the research on outcomes is limited as well. This technique is mostly used when there has been a failed penile inversion and that skin is no longer usable. The only improvement over the penile inversion is that the colon tissue is self-lubricating and will allow the vagina to be self-lubricating as well. Using the penile tissue, the vagina must be artificially lubricated.
Ercolano, A. (2021, January 26)
Pre-Surgery
Like other gender affirming surgeries, insurance requires two, letters of recommendation and 12 months of well documented gender dysphoria prior to surgery. These can be attained through working with a therapist prior to surgery. Plan to continue therapy after surgery to address changes in mood that comes with surgeries of this magnitude. It is also advised to quit smoking up to three months prior to surgery and continue to not smoke for one to three months after surgery. Nicotine is known to reduce the healing process and can increase the time it will take to heal.
Prior to the surgery, skin follicles on the scrotal or penial skin must be removed, if left then there is a possibility of hair growth inside the created vagina. To ensure no hair follicles are left, most prefer scrotal electrolysis, where a small amount of electricity is used to destroy the root of the hair. If left until surgery, some surgeons thin the skin and cauterize the visible hair follicles at the time of surgery.
Post-surgery and care
Recovery period may vary depending on the needs of the patient, though the average time to recover is 6-8 weeks and sexual activity can continue after 12. After the surgery is complete the newly created vagina will be about 4-6 inches deep, though this will vary depending on the size of the patient. Once the patient is finished with the surgery, they will have to dilate the vagina to ensure it continues to hold its shape. For the first few weeks the patient will dilate twice a day for at least 15 minutes, starting with the smallest in the pack. Patients will have to continue dilating, moving up in size as instructed by their care team. Dilation may be uncomfortable but should not be painful, if there is pain try readjusting the dilator and notify your care team. Make sure to use lubrication prior to dilation. Example dilators and sizes are pictured below:

Starting a week after surgery it is important to keep clean and begin douching. Douching once or twice a week should be enough, though this is dependent on the amount of vaginal discharge being experienced. Heaver discharge may require douching more often. After douching, dry the outside of the vagina and focus on keeping the outside clean and dry. Washing in the shower without scrubbing the area.
If you traveled for this surgery, you may be asked to stay in town for at least four weeks after the surgery, with biweekly appointments.
Zero Depth Vaginoplasty
Zero Depth Vaginoplasty (ZDV) is a less invasive way to create the vulva without a vagina. This procedure is one set, and the recovery time is easier, there is no need for dilation and there is less risk for complications such as bladder, urethra, or rectum injuries. There is still a need for two letters of recommendation from mental health providers and the patient must be on HRT for at least a year prior to surgery. After surgery there will be swelling and soreness, it advised to take it easy and not do any strenuous work for 3-4 weeks post-surgery. The drawback for this type of surgery is that it does not allow for penetration sex. However, some may not be concerned for that and this is an easier and quicker option in terms of time spent recovering.
In terms of the surgery itself, it is similar to the vaginoplasty but without the vaginal canal. The phallus and testicles are removed and the construction of the clitoris and labia majora are created in the same way they are for a full depth vaginoplasty. Some surgeons opt to create a shallow vaginal canal but there would still be no need to dilate, and penetrative sex is still not an option with a shallow vaginal canal. The goal is still to preserve sensation and urinary function on the external of the vagina.
Sources
Ercolano, A. (2021, January 26). FAQ: Vaginoplasty: The Johns Hopkins Center for Transgender health. Retrieved February 20, 2021, from https://www.hopkinsmedicine.org/center-transgender-health/services-appointments/faq/vaginoplasty
Meltzer, T., MD. (2016, June 17). Vaginoplasty procedures, complications and aftercare. Retrieved February 20, 2021, from https://transcare.ucsf.edu/guidelines/vaginoplasty
T. (2021). Article: My doctor online. Retrieved February 20, 2021, from https://mydoctor.kaiserpermanente.org/ncal/article/vaginal-dilation-after-vaginoplasty-1290049
T. (2021). Buy soul source grs dilator: The pelvic hub. Retrieved February 20, 2021, from https://www.thepelvichub.com/shop/grs-vaginal-dilators
Ercolano, A. (2021, January 26). FAQ: Vaginoplasty: The Johns Hopkins Center for Transgender health. Retrieved February 21, 2021, from https://www.hopkinsmedicine.org/center-transgender-health/services-appointments/faq/vaginoplasty